Can You Catch Up on Sleep on Weekends? What Sleep Debt Research Actually Says
The honest answer is "partly — but not for the things that matter most." Here's what 2019–2024 research found, and the strategy that beats catch-up sleep entirely.
It's 11 PM on a Friday. You've slept five or six hours each night this week, so you decide you'll catch up on the weekend — no alarm Saturday. You wake at noon, eat lunch, then nap two more hours. By Sunday night you can't fall asleep until 3 AM. Monday morning, in some ways, you feel worse than you did on Friday.
You've probably done this. And the gut sense — that binge-sleeping doesn't quite work — has been increasingly confirmed by precision-instrumentation sleep research published over the last few years.
The short answer. Weekend catch-up sleep partially helps. Drowsiness, mood, and some inflammation markers do recover. But insulin sensitivity, sustained attention, circadian alignment, and long-term mortality risk don't reset in two nights. And once you sleep more than about two hours longer than your weekday baseline, the catch-up actually starts to backfire (Depner 2019; BMJ Open Diabetes Research & Care).
This article covers (1) why "sleep debt" isn't just a metaphor, (2) what actually recovers and what doesn't, (3) how long real recovery takes, (4) why consistency beats catch-up as a strategy, and (5) practical steps if you're already behind.
What "sleep debt" means — and why it's more than a metaphor
"Sleep debt" sounds like wellness marketing, but it's been a quantified concept in sleep medicine since the 1990s. The most cited study is Van Dongen et al., published in SLEEP in 2003.
- 48 healthy adults were limited to 6 hours of sleep per night for 14 days.
- A separate group was kept awake for 88 hours straight as a comparison.
- By day 14, the cognitive performance of the 6-hour group had declined to the same level as two consecutive nights without any sleep.
What was more striking was the self-perception. The 6-hour group didn't notice their own decline. Chronic restriction accumulates while becoming invisible to the person experiencing it. What you read as "I've adapted" is often a measurable deficit you've stopped feeling. (See also Why Am I Tired After 8 Hours of Sleep? for the felt-experience side of this.)
This is what makes "debt" the right metaphor. An hour short each night accumulates like compound interest — you don't see it until later.
The short answer: partly yes, mostly no
Pulling the research together:
| Indicator | Recovers in two weekend nights? |
|---|---|
| Subjective drowsiness | ✓ Mostly recovers |
| Mood / anxiety | ◐ Partially |
| Some inflammation markers | ◐ Partially |
| Sustained attention (vigilance) | ✗ Doesn't recover |
| Insulin sensitivity | ✗ Doesn't recover (can worsen) |
| Circadian phase alignment | ✗ Disrupted |
| Long-term mortality / CV risk | ✗ Inconsistent across studies |
You "feel" recovered because drowsiness and mood are the conscious channels. But the measurable indicators that drive long-term health — especially metabolic and cognitive — don't reset in two nights.
The headline: what you feel and what's actually fixed are different things. The health impact tracks the latter.
What actually recovers — and what doesn't
The most decisive data is from a 2019 Current Biology study by Christopher Depner's group at the University of Colorado Boulder.
- 36 healthy adults were divided into three groups:
- Adequate sleep (control, up to 9 hours)
- Chronic restriction (5 hours every weekday and weekend)
- Restriction + weekend recovery (5 hours weekdays, ad libitum on weekends)
- The study tracked them for 13 days in the lab — a 3-day baseline, 5 weekday nights, 2 weekend nights, then 3 more weekday nights.
The results ran counter to intuition.
- Weight: All three groups gained weight from late-night snacking — and the weekend recovery didn't prevent it.
- Whole-body insulin sensitivity: The chronic restriction group dropped 13%. The weekend recovery group dropped 27% — worse than the group that didn't recover at all.
- Tissue-level insulin sensitivity: Only in the weekend recovery group did muscle insulin sensitivity drop a significant 9%, while hepatic sensitivity fell 23% but didn't quite reach statistical significance (P = 0.054). The chronic restriction group didn't show the same tissue-specific drop — so the tissue-level damage was a signature of the "recovery" group, not the deprived group.
The interpretation: weekend lie-ins push the circadian rhythm forward. The phase shift desynchronizes meal timing from insulin secretion timing, and the same calories cost more metabolically. "Catch up on weekends" can actively increase metabolic harm.
Sustained attention is a separate story. In a study reviewed by Guzzetti & Banks (2023), participants restricted to 4 hours per night for 5 nights then given a single recovery night with 10 hours in bed still didn't fully restore vigilance (reaction time, lapse rate). Other multi-night recovery studies reach the same partial-recovery conclusion. Two nights are simply not enough to reach the bottom of months of cumulative debt.
Some indicators do bounce back — drowsiness, mood, parts of the inflammatory response. The trap is that it feels like total recovery.
How long does real recovery take?
The most cited estimate is one hour of sleep debt requires about four days of recovery (Kitamura et al., 2016, Scientific Reports). With one important caveat — those four days were measured under controlled conditions where participants had a 12-hour sleep opportunity per night. To recover at a normal 7–8 hours of nightly sleep, the timeline stretches substantially longer.
The math:
- Missing one hour every weekday → a weekly debt of about 5 hours
- Recovery in a 12-hour-opportunity setting → about 20 days
- Recovery on normal 7–8 hours → considerably longer
- What two weekend nights can plausibly recover → at most 1–2 hours' worth
These are averages with wide individual variation. But the takeaway holds — two weekend nights are arithmetically insufficient to repay a week's deficit.
The recovery curve is also non-linear. The first night gives the biggest gain. The second night gives roughly half of that. The third about half again. That's why 3–4 nights of solid sleep chip away at accumulated debt more effectively than two marathon weekend sessions.
When catch-up sleep backfires: social jet lag and the two-hour ceiling
How much extra you sleep matters as much as whether you do.
Social jet lag is the mismatch between weekday and weekend sleep midpoints. If you sleep midnight to 6 AM on weekdays (midpoint 3 AM) and 2 AM to noon on weekends (midpoint 7 AM), you're effectively flying through four time zones every weekend — without the airplane. (For reference on actual time zones, see the World Clock.)
A NHANES analysis (N = 23,475) published in BMJ Open Diabetes Research & Care found:
- For people sleeping less than the apparent optimum (~7h 18m) on weekdays, weekend catch-up of about 1–2 hours was associated with better insulin sensitivity.
- Beyond 2 hours, the benefit faded. And for people already at or above the weekday optimum, additional weekend sleep flipped to a negative signal.
In practice:
- Weekday 6h + weekend 7–8h → some recovery signal
- Weekday 6h + weekend 9–10h → benefit gone or reversed
- Weekday 7–8h + weekend 9–10h → metabolic cost
This is why Monday mornings can feel worse: subjectively you slept enough; objectively your circadian clock didn't return to weekday rhythm before the new workweek.
Age and chronotype shift the answer. Åkerstedt et al. (2019, J Sleep Res) found that, under 65, short weekday sleep paired with long weekend sleep partially offset short-sleep mortality risk. Over 65, the protective signal weakened — fragmented older-adult sleep doesn't recover by simple volume.
The most rigorous recent test came from Chaput et al. (2024, SLEEP), which used accelerometer-measured sleep in 73,513 adults over 8 years. Self-reported recovery effects from earlier studies didn't replicate: hazards for all-cause mortality and cardiovascular events for ≥2-hour weekend catch-up were HR 1.17 and 1.05 — no protection.
The honest summary: catch-up isn't necessarily harmful, but it doesn't fix chronic restriction. And the ambiguity itself is the conclusion — catch-up is a side patch, not a solution.
A better strategy: sleep regularity beats catch-up
A 2024 SLEEP paper by Windred et al. shifted the framing. Using 60,977 UK Biobank participants:
- Sleep regularity predicted mortality more strongly than sleep duration.
- The most-regular quintile had 20–48% lower all-cause mortality than the least-regular quintile (the range spans different adjustment models).
In other words — a steady seven hours every night beats a six-hour weekday / nine-hour weekend mix, even if the total matches. That's a slightly uncomfortable result for anyone who's tracked hours but ignored timing.
Two implications:
- The goal isn't enough sleep. It's enough and consistent sleep.
- Catch-up is the consolation prize. The actual fix is a weekday pattern that doesn't accumulate debt.
A consistent bedtime helps make this concrete. If 7 AM is the wake target, going to bed at roughly the same time on Friday, Saturday, and Sunday as on Monday is the single most effective lever — and it's how you escape the four-time-zone weekend. (Cycle-aligned bedtimes for any wake time are mapped out in What Time Should I Go to Bed if I Wake Up at 6 AM?; the 90-minute sleep cycle covers why end-of-cycle wakes feel so different.)
If you're already behind: practical tips
Total recovery is hard. Avoiding additional accumulation is the high-leverage move.
- Move weekday bedtime forward by 15–20 minutes at a time. Not an hour all at once — small shifts let the circadian rhythm catch up.
- Cap Saturday lie-ins to 1 hour past your usual wake time. Beyond that, social jet lag accrues.
- Skip marathon naps. Anything longer than two hours interferes with that night's sleep. A 20–30 minute nap reduces drowsiness most efficiently — though full vigilance recovery from naps is limited (MSU 2021).
- Light and caffeine timing. 30 minutes of natural light right after waking, no caffeine after early afternoon. Mundane advice, but it's the most reliable lever for circadian alignment. (For longer-window focus and circadian crossover, see The Science Behind the Pomodoro Technique.)
- Make when you sleep as consistent as how much. The Windred 2024 takeaway — same bedtime and wake time most days beats catching up.
Preventing debt is dramatically more efficient than recovering from it. And prevention is mostly about clock position, not clock total — going to bed at roughly the same time every night.
Your target hours by age (the upstream question to all of this) are summarized in How Many Hours of Sleep Do You Need by Age?. Once you have a target, finding "what time, exactly?" — for any wake target — is a 90-minute cycle calculation. Doing it by hand isn't necessary.
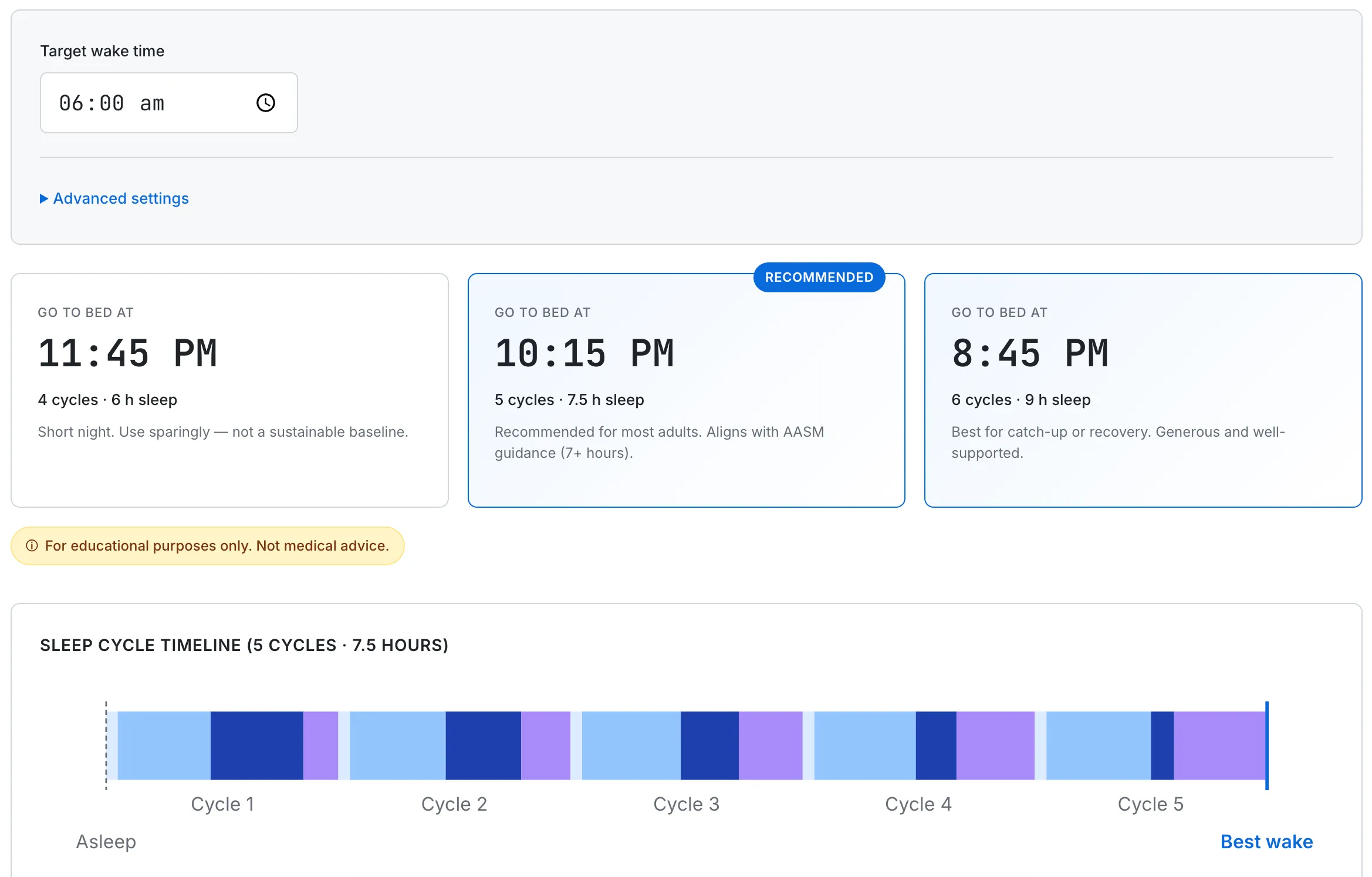
A consistent bedtime and wake time, even across the weekend, is a stronger health signal than weekend catch-up sleep (Windred et al., 2024). The calculator finds the cycle-aligned window for whatever wake time you set.
This guide summarizes peer-reviewed sleep research and is for educational use only. Individual sleep needs and recovery dynamics vary, and the studies cited used controlled lab conditions or population-level cohorts, not personalized predictions. None of this is medical advice or a substitute for a clinical evaluation. If you have ongoing trouble sleeping, suspect a sleep disorder, or have concerns about persistent fatigue, please consult a licensed healthcare professional.